Introduction
Gastrointestinal (GI) strictures—narrowings in the digestive tract—can cause pain, difficulty swallowing, bloating, or bowel obstruction. While these symptoms can severely affect daily life, modern medicine offers effective solutions. One of the most common and minimally invasive treatments is endoscopic dilatation.
At Dr. Deetlefs’s practice, patients with strictures due to conditions like Crohn’s disease, ulcerative colitis, or scar tissue from surgery can benefit from this procedure.
In this article, we explain everything you need to know about endoscopic dilatation, including what it is, how it works, preparation, recovery, and potential risks.
What Are Gastrointestinal Strictures?
A GI stricture is an abnormal narrowing of a section of the digestive tract. Strictures can occur in the:
- Esophagus – leading to difficulty swallowing (dysphagia)
- Stomach or duodenum – causing nausea, vomiting, and bloating
- Small or large intestine – leading to constipation, cramping, or partial obstruction
Common Causes
- Inflammatory bowel disease (IBD)
- Crohn’s disease is a leading cause of strictures in the small and large intestines
- Chronic inflammation leads to scar tissue formation
- Surgical scarring
- Post-operative adhesions may narrow sections of the gut
- Radiation therapy
- Can cause tissue scarring in patients treated for abdominal cancers
- Esophageal conditions
- GERD, eosinophilic esophagitis, or acid reflux can lead to esophageal strictures
- Tumors or polyps
- Less commonly, strictures are caused by abnormal growths
What Is Endoscopic Dilatation?
Endoscopic dilatation is a procedure used to widen narrowed sections of the gastrointestinal tract using specialized tools inserted via an endoscope.
The goal is to relieve obstruction, improve swallowing, or restore normal bowel function without the need for major surgery.
Key advantages include:
- Minimally invasive
- Performed on an outpatient basis
- Reduces recovery time compared to surgery
- Can be repeated if strictures recur
How Does the Procedure Work?
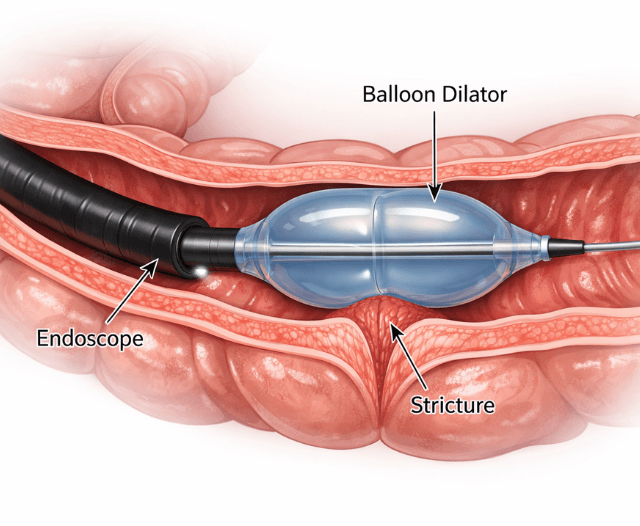
Endoscopic dilatation uses either balloon dilators or bougie dilators to gently expand the narrowed area.
Step-by-Step Process
- Sedation and preparation
- The patient receives sedation or anesthesia
- Positioning depends on the stricture location
- Insertion of the endoscope
- A flexible tube with a camera allows the gastroenterologist to visualize the stricture
- This ensures precise placement of the dilator
- Dilatation
- Balloon dilator: Inflated gradually at the site of the narrowing to stretch the tissue
- Bougie dilator: A tapered instrument gently passed through the stricture
- Assessment
- The stricture is reassessed after dilation
- Multiple passes may be necessary for severe narrowing
- Completion
- The endoscope is removed
- The patient is monitored briefly before discharge
Endoscopic dilatation is generally safe and effective, with most patients experiencing immediate relief of symptoms.
Who Can Benefit from Endoscopic Dilatation?
Patients with GI strictures caused by:
- Crohn’s disease or ulcerative colitis
- Post-surgical scar tissue
- Esophageal narrowing due to GERD or radiation
- Benign strictures
Symptoms that may indicate the need for dilatation include:
- Difficulty swallowing or sensation of food sticking
- Abdominal pain, bloating, or constipation
- Vomiting or nausea
- Weight loss due to poor intake
Preparation for Endoscopic Dilatation
Preparation varies depending on the stricture location:
Esophageal Strictures
- Fasting: Typically 6–8 hours before the procedure
- Medication review: Blood thinners or other medications may need temporary adjustment
- Sedation plan: Discuss anesthesia options with your gastroenterologist
Intestinal Strictures
- Bowel prep: Cleansing solution may be required for colon or small intestine strictures
- Dietary instructions: Clear liquids prior to the procedure
- Medication review: Especially important for patients with IBD
Preparation is critical for safety, visibility, and optimal results.
Recovery After Endoscopic Dilatation
Most patients can return home the same day. Recovery depends on the stricture location and severity.
Immediate Recovery
- Observation for 1–2 hours post-procedure
- Mild discomfort, cramping, or bloating may occur
- Resume clear fluids initially, then gradually progress to regular diet
Short-Term Recovery Tips
- Eat soft foods for the first few days
- Avoid hard, crunchy, or sticky foods that may irritate the treated area
- Stay hydrated
Follow-Up
- Gastroenterologist may schedule a follow-up endoscopy
- Multiple dilatations may be necessary if strictures recur
- Continuous monitoring for patients with IBD is recommended
Risks and Complications
Endoscopic dilatation is minimally invasive, but potential risks include:
- Perforation of the GI tract (rare)
- Bleeding at the dilation site
- Infection (uncommon)
- Recurrence of the stricture
The procedure is considered safe when performed by an experienced gastroenterologist. Discuss all concerns with your doctor before treatment.
Advantages Over Surgery
Endoscopic dilatation offers multiple benefits compared to surgical intervention:
- Minimally invasive – no large abdominal incisions
- Short recovery time – most patients resume normal activities within days
- Lower risk of complications – less bleeding and infection risk
- Repeatable – can be performed multiple times if strictures recur
Surgery may be reserved for severe or complicated strictures that do not respond to endoscopic treatment.
Success Rates and Effectiveness
- Success rates vary depending on stricture length, location, and underlying cause
- For short, simple strictures, relief is immediate and long-lasting
- In patients with Crohn’s disease, multiple sessions may be required due to chronic inflammation
Studies indicate that endoscopic dilatation is highly effective in improving quality of life and preventing obstruction without the need for major surgery (ACG Guidelines).
When to Seek Immediate Medical Attention
After the procedure, contact your gastroenterologist if you experience:
- Severe abdominal pain
- Vomiting
- Fever or chills
- Significant bleeding
- Difficulty swallowing or passing stools
Early attention ensures prompt management of any complications.
Long-Term Management After Endoscopic Dilatation
While endoscopic dilatation provides immediate relief from GI strictures, long-term management is crucial to prevent recurrence.
Patients with conditions like Crohn’s disease or ulcerative colitis should work closely with their gastroenterologist to monitor inflammation, maintain remission, and adjust medications as needed.
Nutritional support is also essential—patients may need a diet rich in easily digestible foods, adequate hydration, and supplementation if malabsorption is present.
Additionally, regular follow-up endoscopies or imaging studies may be recommended to detect early signs of stricture recurrence and address them promptly.
Incorporating lifestyle measures such as stress management, avoiding smoking, and following a tailored anti-inflammatory diet can further improve outcomes and support long-term digestive health.
Conclusion
Endoscopic dilatation is a safe, effective, and minimally invasive treatment for gastrointestinal strictures. By widening narrowed areas of the digestive tract, it restores normal function, alleviates symptoms, and can prevent the need for more invasive surgery.
At Dr. Deetlefs’s clinic, we specialize in diagnosing strictures, performing endoscopic dilatation, and managing long-term digestive health.
If you experience difficulty swallowing, persistent bloating, or intestinal obstruction symptoms, don’t wait—early evaluation can improve outcomes and quality of life.
Contact Dr. Deetlefs
If you are experiencing symptoms of a GI stricture, book a consultation with Dr. Deetlefs today.
Take control of your digestive health with expert, minimally invasive care.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.