Polypectomy: The Key to Preventing Colorectal Cancer and Why It Matters
Colorectal cancer is one of the most common cancers worldwide, but it is also one of the most preventable. One of the most effective ways to reduce the risk of developing colorectal cancer is through polypectomy, a procedure that removes polyps from the colon or rectum.
Since most colorectal cancers develop from precancerous polyps, early detection and removal can significantly lower the chances of the disease progressing.
If you or a loved one has been advised to undergo a polypectomy, understanding the procedure and its benefits can help ease any concerns.
This article explores what a polypectomy is, how it is performed, its role in cancer prevention, and what to expect before and after the procedure.
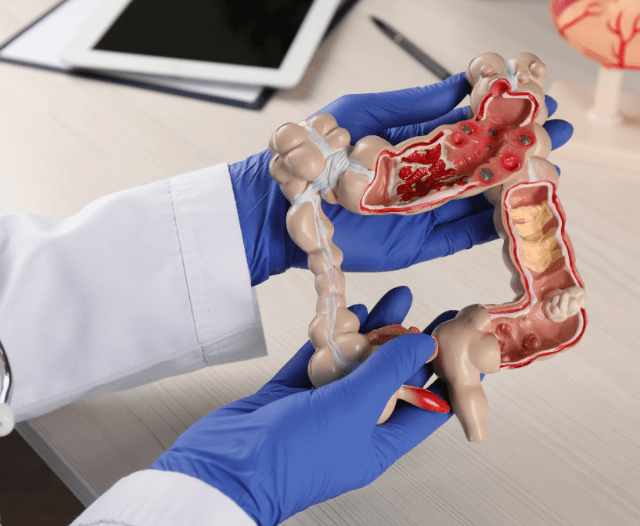
What Are Polyps and Why Are They a Concern?
Polyps are abnormal growths that develop on the inner lining of the colon or rectum.
While most polyps are benign (noncancerous), some have the potential to become cancerous over time. These growths can vary in shape and size and are often classified into different types:
Types of Polyps
- Adenomatous Polyps (Adenomas)
These are the most common precancerous polyps. While not all adenomas turn into cancer, they have a higher risk of becoming malignant if left untreated. - Hyperplastic Polyps and Inflammatory Polyps
These types of polyps are generally not precancerous and have a lower risk of developing into colorectal cancer. - Serrated Polyps
Some serrated polyps, particularly large ones, may carry a significant risk of cancer development.
Since polyps do not typically cause symptoms, most people are unaware they have them until they undergo a colonoscopy—a screening test for colorectal cancer.
This is why regular screenings and polyp removal are crucial for prevention.

What Is a Polypectomy?
A polypectomy is a medical procedure used to remove polyps from the colon or rectum. It is commonly performed during a colonoscopy or sigmoidoscopy, both of which use a flexible tube with a camera to examine the digestive tract.
By removing polyps before they have the chance to become cancerous, a polypectomy is considered one of the most effective ways to prevent colorectal cancer.
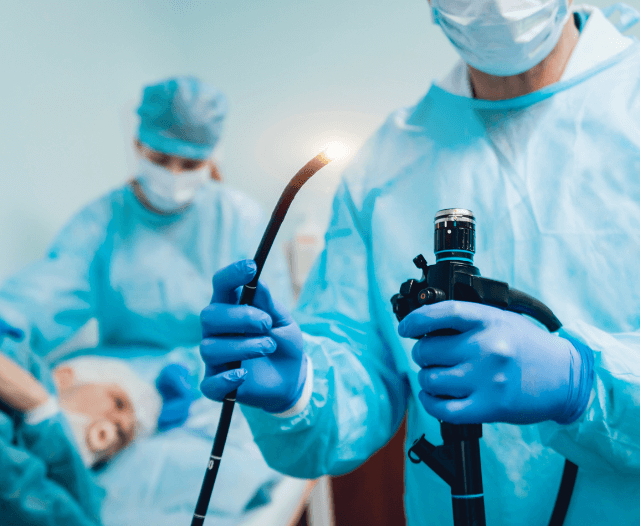
How Is a Polypectomy Performed?
A polypectomy is a minimally invasive procedure performed during a routine colonoscopy. Here’s what to expect during the process:
- Preparation for the Procedure
- Before the colonoscopy, you will need to cleanse your colon using a bowel preparation solution. This ensures a clear view of the colon, making it easier to detect and remove any polyps.
- You may be advised to avoid certain medications (such as blood thinners) before the procedure.
- The Procedure
- A colonoscope (a thin, flexible tube with a camera) is inserted into the rectum and guided through the colon.
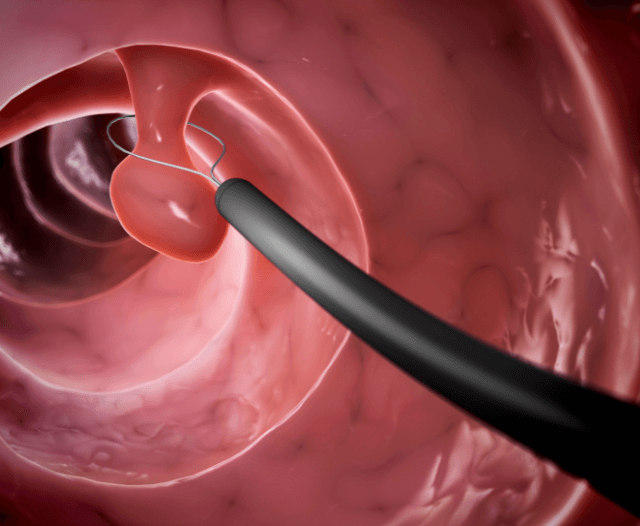
- If a polyp is detected, the doctor will remove it using one of the following methods:
Snare Polypectomy – A wire loop is used to cut off the polyp, often with the help of electrical current (cauterization) to prevent bleeding.
Cold Forceps Polypectomy – Small polyps are removed using forceps without cauterization.
Endoscopic Mucosal Resection (EMR) – Larger polyps may require saline injection to lift the polyp before removal.
- Post-Procedure Recovery
- The entire colonoscopy, including polypectomy, typically takes 20 to 60 minutes.
- You may experience mild bloating or gas after the procedure, but this usually resolves within a few hours.
- Most patients can resume normal activities the next day.

Why Is a Polypectomy Important for Colorectal Cancer Prevention?
The significance of a polypectomy lies in its ability to remove precancerous polyps before they turn into cancer.
Studies show that patients who undergo routine colonoscopies with polypectomy have a significantly lower risk of developing colorectal cancer.
Key Benefits of Polypectomy in Cancer Prevention
- Early Detection and Removal – Identifying and removing polyps in their early stages prevents cancer from developing.
- Reduces Risk of Invasive Cancer Treatment – If cancerous polyps are detected early, they can be removed without the need for chemotherapy or surgery.
- Improves Long-Term Health Outcomes – Regular screenings and polypectomy help maintain a healthy colon and reduce the risk of complications later in life.
Who Should Get a Polypectomy?
- Individuals Over 45
- Those with a Family History of Colorectal Cancer
- Patients with Symptoms of Colorectal Issues
Although polyps are often asymptomatic, some people may experience:
- Rectal bleeding
- Changes in bowel habits
- Unexplained abdominal pain
What to Expect After a Polypectomy
Recovery Period
- Most people can go home the same day after a polypectomy.
- You may have mild discomfort, bloating, or light rectal bleeding, which should resolve within a few days.
- Avoid heavy lifting and strenuous exercise for at least 24 hours after the procedure.
Follow-Up Care
- The removed polyps will be sent to a pathology lab to determine whether they are benign, precancerous, or cancerous.
- Your doctor will inform you if additional treatment or more frequent screenings are necessary.
- If multiple polyps are found, you may need more frequent colonoscopies (e.g., every 3-5 years instead of every 10 years).
Common Concerns About Polypectomy
1. Is a Polypectomy Painful?
- The procedure is performed under sedation, so you won’t feel discomfort during the process.
2. Are There Risks Involved?
- A polypectomy is a very safe procedure. However, like any medical intervention, there are some risks, including:– Minor bleeding (usually resolves on its own)
– Perforation of the colon (very rare, but requires medical attention)
- Can Polyps Grow Back After Removal?
- Once removed, a polyp cannot regrow, but new ones can develop over time.
This is why routine screenings are important.
How to Reduce the Risk of Developing Polyps
While polypectomy effectively removes polyps, prevention is the best strategy to reduce the chances of new polyps forming.
Here’s how you can take control of your colorectal health:
Eat a High-Fiber Diet
- Fiber-rich foods (vegetables, fruits, whole grains) promote healthy digestion and reduce polyp formation.
- Aim for at least 25-30 grams of fiber daily.
Limit Processed Meats and Red Meat
- Diets high in processed meats (bacon, hot dogs, sausage) and excessive red meat are linked to an increased risk of polyps and colorectal cancer.
- Opt for lean protein sources like fish, poultry, and plant-based proteins.
Exercise Regularly
- Staying active reduces inflammation in the body and helps maintain a healthy gut.
- Aim for 150 minutes of moderate exercise per week (e.g., brisk walking, cycling).
Maintain a Healthy Weight
- Obesity is a risk factor for polyps and colorectal cancer.
- Keeping a healthy body weight reduces your risk of developing precancerous growths.
Avoid Smoking and Excessive Alcohol
- Smoking and heavy alcohol consumption increase the risk of colorectal cancer.
- If you smoke, quitting significantly lowers your risk.
Consider Genetic Testing if You Have a Family History
- If colorectal cancer runs in your family, talk to your doctor about genetic screening and earlier testing.
- Conditions like Lynch syndrome or familial adenomatous polyposis (FAP) may require more frequent screenings.

Conclusion
A polypectomy is a life-saving procedure that significantly reduces the risk of colorectal cancer. By removing precancerous polyps early, you can prevent cancer before it even starts.
If you’re over 45 years old, have a family history of colorectal cancer, or experience digestive symptoms, scheduling a colonoscopy and polypectomy can protect your health.
Early detection saves lives—don’t wait until symptoms appear. If your doctor recommends a polypectomy, know that it is a safe, effective, and essential step in maintaining your gastrointestinal health.
Get in Contact with Dr. Deetlefs
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.