Endoscopic Haemostasis: A Key to Managing Bleeding Lesions
Introduction
The medical field has experienced significant advancements in terms of diagnostic and therapeutic procedures.
One of the revolutionary advancements has been the advent of endoscopy, which allows direct visualization and treatment of internal structures.
When it comes to the management of gastrointestinal (GI) bleeding, endoscopic haemostasis has emerged as a crucial intervention.
This article aims to shed light on endoscopic haemostasis and its role in managing bleeding lesions.
Understanding Endoscopic Haemostasis
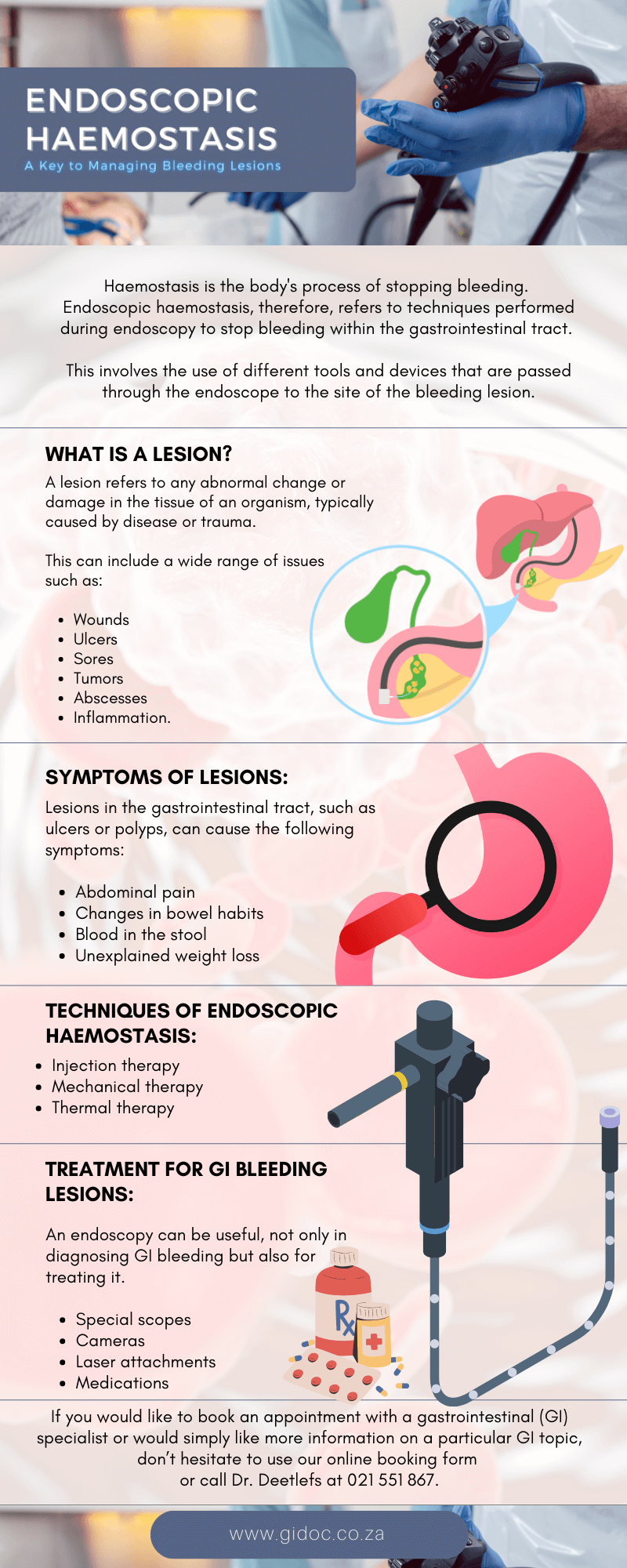
Haemostasis is the body’s process of stopping bleeding.
Endoscopic haemostasis, therefore, refers to techniques performed during endoscopy to stop bleeding within the gastrointestinal tract.
This involves the use of different tools and devices that are passed through the endoscope to the site of the bleeding lesion.
The management of GI bleeding has evolved over the years with endoscopic haemostasis becoming the cornerstone of therapy.
The primary goal is not only to stop active bleeding but also to prevent rebleeding.

What is a Lesion?
A lesion refers to any abnormal change or damage in the tissue of an organism, typically caused by disease or trauma. This can include a wide range of issues such as wounds, ulcers, sores, tumors, abscesses, and areas of inflammation.
In the context of medical imaging, a lesion might be an area of tissue that has been damaged due to injury or disease, which could include cancer or infections.
This term does not indicate a specific type of tissue change or damage but is rather a broad term that can refer to a variety of issues.
The exact characteristics and implications of a lesion can greatly vary depending on factors such as the location, size, and cause of the lesion.
Some lesions may cause pain or discomfort, while others might be completely asymptomatic. Certain lesions can be easily identified through a physical examination, while others may require advanced imaging techniques for detection.
Symptoms of Lesions:
Lesions in the gastrointestinal tract, such as ulcers or polyps, can cause the following symptoms:
- Abdominal pain
- Changes in bowel habits
- Blood in the stool
- Unexplained weight loss

Techniques of Endoscopic Haemostasis
The choice of haemostasis technique largely depends on the location and nature of the bleeding lesion.
However, most procedures fall under one of three categories: injection therapy, mechanical therapy, and thermal therapy.
Injection Therapy: This involves injecting a solution, such as adrenaline, directly into or around the bleeding vessel to constrict it and stop the bleeding.
Mechanical Therapy: This includes methods like band ligation or clip placement, where the bleeding vessel is physically closed off to stop the bleeding.
Thermal Therapy: Here, heat is applied to the bleeding site to coagulate the blood and stop the bleeding. Examples include argon plasma coagulation and electrocoagulation.
All these methods can be used alone or in combination, depending on the situation and the judgement of the endoscopist.
Treatment for GI Bleeding Lesions
An endoscopy can be useful, not only in diagnosing GI bleeding but also for treating it.
The treatment is called haemostasis of bleeding lesions and the idea is to stop the bleeding.
The use of special scopes with cameras and laser attachments, along with medications can be used to stop the bleeding.
In addition, your doctor can use tools alongside scopes to apply clips to the bleeding vessels to stop the bleeding.
If hemorrhoids are the cause of your bleeding, over the counter (OTC) treatments might work for you.
If you find that OTC remedies don’t work, your doctor might use a heat treatment to shrink your hemorrhoids.
If infection is the cause, then the doctor might prescribe antibiotics which are usually enough to treat infections.

The Role of Endoscopic Haemostasis in Managing Bleeding Lesions
GI bleeding can be a life-threatening emergency, and rapid assessment and treatment are vital.
Endoscopic haemostasis is often the first line of treatment due to its high success rate, minimal invasiveness, and relatively low risk of complications.
Several types of bleeding lesions can be managed through endoscopic haemostasis. These include bleeding peptic ulcers, varices, angiodysplasia, and post-polypectomy bleeding.
For example, in the case of bleeding peptic ulcers, endoscopic haemostasis can achieve initial haemostasis in more than 90% of cases.
If the bleeding is from varices (abnormally dilated vessels), band ligation or sclerotherapy can be effectively used.
Limitations and Risks
While endoscopic haemostasis is a key intervention, it is not without its limitations and risks.
Complications, although rare, can occur. These can include perforation, infection, and, in the case of variceal band ligation, stricture formation.
There are also situations where endoscopic haemostasis may not be successful, such as in the presence of coagulopathy (a condition affecting the blood’s ability to clot).
In such cases, alternative or additional treatments such as radiological intervention or surgery may be needed.
Advancements in Endoscopic Haemostasis recent advancements in technology have led to the development of new devices and techniques that have improved the efficacy and safety of endoscopic haemostasis.
These include over-the-scope clips, haemostatic powders, and endoscopic suturing devices. These novel tools are broadening the scope and effectiveness of endoscopic haemostasis and providing physicians with a wider array of options to manage bleeding lesions.
Over-the-Scope Clips (OTSC):
Over-the-scope clips are larger than standard clips and are able to close larger defects and exert a higher compressive force. This has made them particularly effective in managing more substantial bleeding and deeper lesions. They are also highly beneficial in preventing rebleeding.
Haemostatic Powders:
Haemostatic powders are a relatively new innovation. These powders, when applied to a bleeding site, absorb water from the blood, concentrate the clotting factors, and help in the formation of a stable clot. They are particularly effective in managing diffuse bleeding and have shown excellent results in acute, non-variceal upper GI bleeding.
Endoscopic Suturing Devices:
These are innovative devices that enable physicians to stitch from within the GI tract, thus providing a new method to achieve haemostasis. While still not extensively used due to technical complexity, these devices offer an excellent non-surgical option for haemostasis in challenging scenarios.
Conclusion
Endoscopic haemostasis has undoubtedly become a cornerstone in the management of gastrointestinal bleeding.
The evolution of this field has resulted in a shift from more invasive procedures to minimally invasive endoscopic techniques, improving patient outcomes and recovery times. With the development of advanced tools and techniques, the capabilities of endoscopic haemostasis are continually expanding, thus offering more effective solutions for the management of bleeding lesions.
However, each case of GI bleeding is unique, and a successful outcome often depends on a combination of the endoscopist’s skill, the choice of technique, and individual patient factors.
As we move forward, further advancements in this field will undoubtedly provide even more efficient and safer methods of managing GI bleeding.
Gi Doc Cape Town is a practice founded to provide medical solutions in the area of gastroenterology.
Over the years, Dr Eduan Deetlefs has earned the reputation of a trusted health expert providing consultative, diagnostic, and therapeutic endoscopic and related services to patients in
Cape Town and beyond.
Dr Deetlefs has admitting rights and performs endoscopies at both Mediclinic Milnerton and Life Vincent Pallotti Hospitals.
Services include consultations for gastrointestinal and liver related diseases with a specific interest in inflammatory bowel disease and iron deficiency anaemia caused by obscure gastrointestinal bleeding.
He furthermore performs numerous more specialised procedures such as capsule endoscopy, double-balloon enteroscopy, ERCP and various interventional procedures including polypectomies for large polyps, haemostasis of bleeding lesions, ablation of Barrett’s oesophagus and placement of feeding tubes (PEG).
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form
or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.