The Digestive Detective: Gastroscopy’s Role in Identifying Gastrointestinal Issues
Introduction
The human body is a complex and intricate system, with the digestive tract playing a central role in maintaining overall health.
Sometimes, however, this intricate system can encounter problems that remain hidden beneath the surface. This is where gastroscopy, often referred to as the “digestive detective,” steps in.
In this article, we’ll embark on a journey into the world of gastroscopy, exploring how it acts as a powerful tool in identifying a wide range of gastrointestinal issues.
Gastroscopy Unveiled: The Basics
Gastroscopy, also known as upper gastrointestinal endoscopy, is a minimally invasive procedure used to examine the upper digestive tract.
This includes the esophagus, stomach, and the duodenum – the initial part of the small intestine.
The procedure involves a slender, flexible tube called an endoscope, equipped with a camera and light source at its tip.
The endoscope is gently inserted through the mouth and guided down the throat, allowing healthcare professionals to obtain clear and real-time images of the digestive tract’s interior.

The Multifaceted Role of Gastroscopy
Gastroscopy serves as a versatile tool with several vital roles in the realm of digestive health:
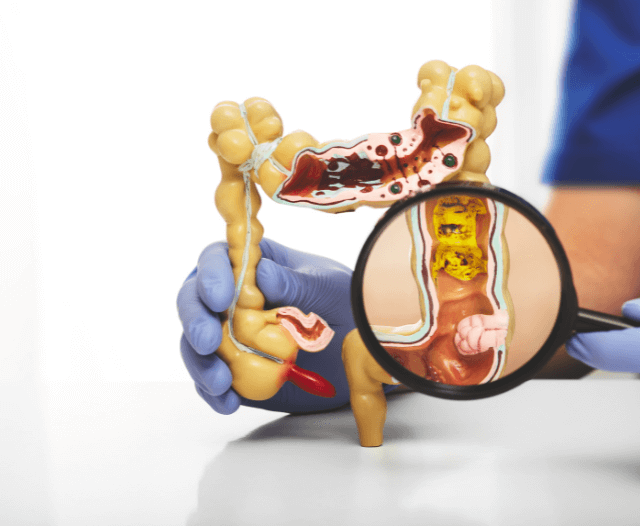
- Uncovering the Unseen: Gastroscopy is particularly valuable when it comes to identifying gastrointestinal issues that might not be apparent through external examinations. It allows healthcare providers to directly visualize the linings of the esophagus, stomach, and duodenum, identifying abnormalities that might be causing discomfort or concern.
- Diagnosing and Confirming Conditions: Gastroscopy plays a pivotal role in diagnosing various gastrointestinal conditions. From detecting ulcers, inflammation, and infections to identifying the presence of conditions like gastritis, celiac disease, and even certain types of cancer, gastroscopy’s images provide a clear window into the health of the digestive tract.
- Investigating Symptoms: Individuals experiencing symptoms such as persistent heartburn, difficulty swallowing, unexplained weight loss, or gastrointestinal bleeding can benefit greatly from gastroscopy. The procedure allows healthcare professionals to investigate the root cause of these symptoms and tailor appropriate treatment plans.
- Guiding Treatment and Intervention: Gastroscopy doesn’t stop at diagnosis. In fact, it often guides treatment strategies. For instance, if a suspicious growth or abnormality is identified, biopsies can be taken through the endoscope. Additionally, certain interventions, such as removing polyps or controlling bleeding, can be performed during the procedure.
- Screening for High-Risk Individuals: For individuals at a higher risk of developing gastrointestinal issues – such as those with a family history of certain conditions or chronic digestive disorders – gastroscopy can serve as a valuable screening tool. Detecting issues early can lead to better outcomes and more effective management.
A Closer Look at the Procedure
Undergoing a gastroscopy is generally a straightforward process:
- Preparation: Before the procedure, patients are often instructed to fast for a certain period to ensure a clear view of the digestive tract. This fasting period allows for accurate imaging and reduces the risk of complications during the procedure.
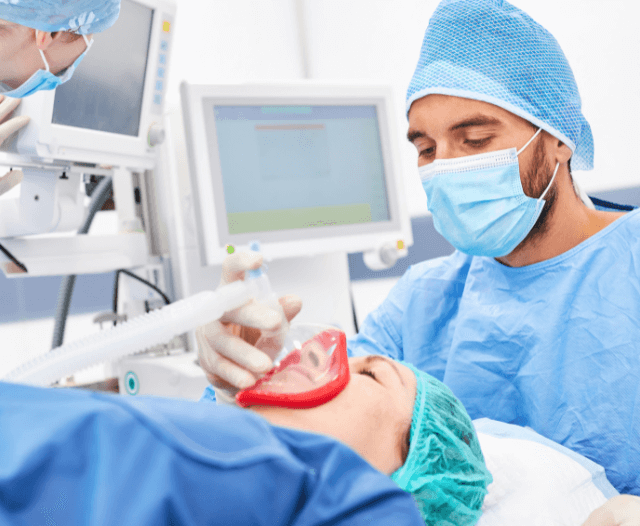
- Anesthesia: Most gastroscopies involve the use of sedation or anesthesia to ensure patient comfort. While the procedure itself is not painful, the sedation helps prevent discomfort or anxiety.
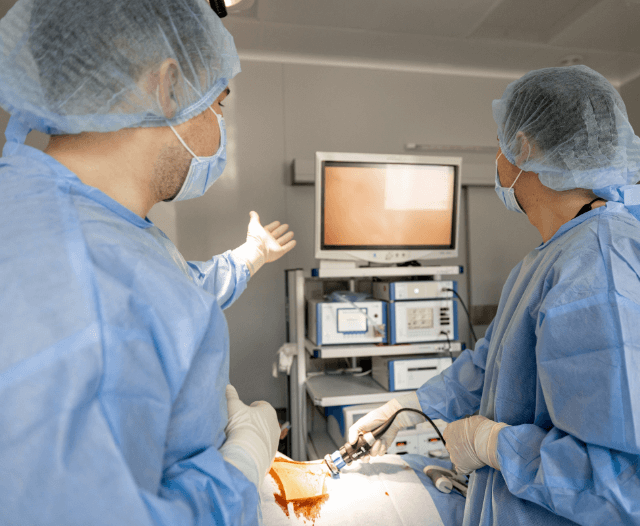
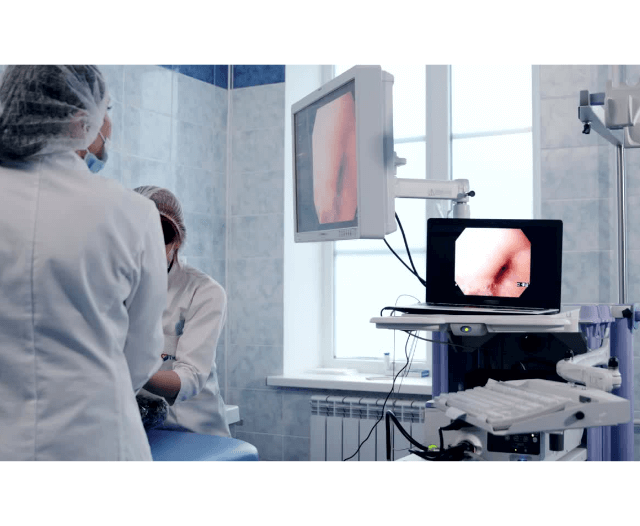
- Procedure: The endoscope is inserted through the mouth and gently guided through the esophagus and into the stomach and duodenum. The camera at the endoscope’s tip captures images that are displayed on a monitor, allowing healthcare professionals to examine the digestive tract in real time.
- Biopsies and Interventions: If necessary, biopsies can be taken during the procedure. These samples are then sent to a laboratory for analysis. Additionally, certain interventions can be performed to address any identified issues.
- Recovery: After the procedure, patients are monitored until the effects of the sedation wear off. It’s advisable to have someone accompany you to the procedure, as the sedation might temporarily impair coordination and judgment.

Empowering Digestive Health Through Knowledge
In the realm of health, knowledge is power.
Gastroscopy exemplifies this principle by providing healthcare providers with the tools they need to accurately diagnose and address a wide array of gastrointestinal issues.
Whether it’s confirming a suspected condition, investigating mysterious symptoms, or simply ensuring the digestive system’s well-being, gastroscopy stands as a reliable ally in the quest for optimal health.
For individuals experiencing persistent digestive discomfort, unexplained symptoms, or those at risk of gastrointestinal issues, consulting with a healthcare professional about the potential benefits of gastroscopy is a proactive step.
The “digestive detective” can unveil answers, provide clarity, and pave the way for effective treatments – ultimately contributing to a healthier and more comfortable life journey.
Gastroscopy Pros and Cons: Weighing the Benefits and Considerations
Gastroscopy, also known as upper gastrointestinal endoscopy, is a valuable medical procedure that provides direct visualization of the upper digestive tract.
Like any medical procedure, it comes with its own set of advantages and considerations.
In this article, we’ll explore the pros and cons of gastroscopy to help you make an informed decision if you’re considering this procedure.
Pros of Gastroscopy:
- Accurate Diagnosis: Gastroscopy allows healthcare professionals to directly view the esophagus, stomach, and duodenum. This real-time imaging aids in accurate diagnosis of various gastrointestinal conditions, including ulcers, inflammation, tumors, and more.
- Early Detection: Gastroscopy plays a vital role in the early detection of gastrointestinal cancers, such as stomach cancer. Detecting these conditions at an early stage significantly improves treatment outcomes.
- Guided Biopsies: If abnormalities are detected, biopsies can be taken during the procedure. These samples help confirm diagnoses and guide treatment strategies, ensuring that appropriate interventions are undertaken.
- Minimally Invasive: Gastroscopy is a minimally invasive procedure that avoids the need for surgical incisions. The endoscope is inserted through the mouth, eliminating the need for external cuts.
- Quick Procedure: The procedure is usually quick, typically lasting between 15 to 30 minutes. This means minimal disruption to your day and relatively shorter recovery time.
- Same-Day Recovery: In most cases, patients can go home on the same day after the effects of sedation wear off. Recovery time is relatively short, and most individuals can resume their normal activities within a day or two.
- Therapeutic Interventions: Gastroscopy not only diagnoses but can also treat certain conditions.During the procedure, polyps can be removed, bleeding can be controlled, and narrow areas of the digestive tract can be dilated.
Cons of Gastroscopy:
- Discomfort and Sedation: While discomfort during the procedure is minimal, some individuals may experience a gagging sensation as the endoscope is inserted. Sedation or anesthesia is used to mitigate this discomfort, but there might be risks associated with sedation.
- Risks of Complications: Like any medical procedure, there are risks of complications. These can include bleeding, infection, perforation (a rare occurrence), or adverse reactions to sedation.
- Preparation and Fasting: Patients typically need to fast before the procedure to ensure a clear view of the digestive tract. Fasting can be inconvenient and uncomfortable for some individuals.
- Post-Procedure Effects: After the procedure, you might experience temporary effects of
sedation, such as drowsiness, impaired coordination, and mild discomfort in the throat. - Cost: Depending on your location and healthcare system, the cost of a gastroscopy can vary. It’s important to check with your healthcare provider and insurance to understand the financial aspects.
- Invasive Nature: While considered minimally invasive, the procedure still involves inserting a foreign object into the body. Some individuals might find this invasive nature unsettling.
Conclusion: Making an Informed Decision
Like any medical procedure, it’s important to weigh the pros and cons of gastroscopy based on your individual health situation and needs.
If you’re experiencing persistent gastrointestinal symptoms, have a family history of gastrointestinal issues, or need further investigation into your digestive health, consulting with a healthcare professional is crucial.
They can provide tailored advice, address your concerns, and guide you toward the best decision for your health and well-being.

Get In Touch with the Expert
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form
or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.