Exploring ERCP: A Comprehensive Guide
This versatile and powerful procedure has revolutionized the field of gastroenterology, allowing healthcare professionals to diagnose and treat a wide range of conditions affecting the bile ducts, pancreas, and gallbladder.
In this comprehensive guide, we will delve into the world of ERCP, exploring its uses, benefits, procedure, potential risks, and much more.
Understanding ERCP: What Is It?
Endoscopic Retrograde Cholangiopancreatography (ERCP) is a specialized medical procedure that combines endoscopy and fluoroscopy to diagnose and treat conditions in the bile ducts, pancreas, and gallbladder.
It provides detailed images and, if necessary, allows for the performance of therapeutic interventions. ERCP is typically performed by a gastroenterologist, a specialist in digestive diseases.
The Key Components of ERCP
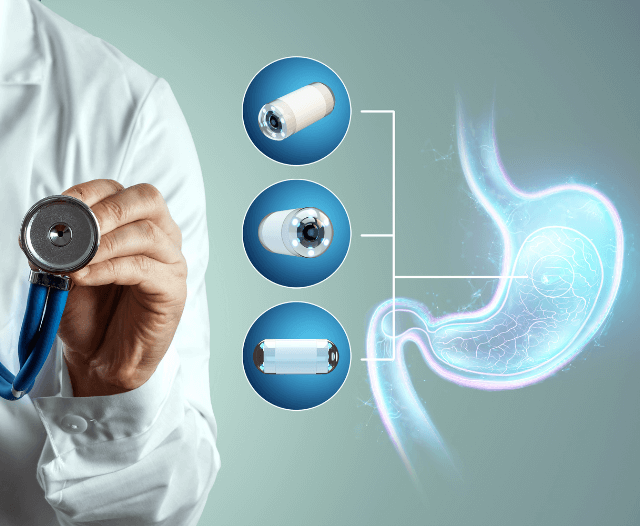
Endoscope: An endoscope is a flexible, tube-like instrument equipped with a light source and a camera. It is inserted through the mouth, down the esophagus, and into the stomach and duodenum (the first part of the small intestine).
Fluoroscopy: Fluoroscopy is a real-time X-ray imaging technique that provides dynamic images of the bile ducts and pancreatic duct.
Contrast Medium: A contrast medium, often a special dye, is injected into the ducts to make them visible on X-ray images.

When Is ERCP Used?
ERCP is employed for various diagnostic and therapeutic purposes, primarily related to the digestive system. Some common indications for ERCP include:
- Diagnosing and Treating Gallstones:
ERCP can identify gallstones trapped in the bile ducts, causing symptoms like jaundice, abdominal pain, and pancreatitis (inflammation of the pancreas). In such cases, the stones can be removed during the procedure.
- Diagnosing and Managing Biliary and Pancreatic Tumors:
ERCP can help in evaluating and diagnosing tumors or strictures (narrowing) in the bile ducts or pancreatic duct. It can also assist in placing stents to relieve blockages caused by these conditions.
- Treating Pancreatitis:
In some cases of acute pancreatitis, ERCP may be performed to remove obstructions or perform other therapeutic procedures.
- Draining Fluid Collections:
ERCP can be used to drain fluid collections (pseudocysts) in the pancreas or bile ducts.
- Evaluating Chronic Abdominal Pain:
When the cause of chronic abdominal pain is unclear, ERCP can be used as a diagnostic tool to explore the pancreas and bile ducts.
- Roux-en-Y Gastric Bypass Procedures:
In patients who have previously undergone gastric bypass surgery, ERCP can be challenging. However, specialized techniques, such as laparoscopy-assisted or double-balloon-assisted ERCP, have been developed to access the desired areas.

The ERCP Procedure: What to Expect
Before undergoing ERCP, patients are typically given instructions about fasting to ensure an empty stomach. The procedure is performed in a hospital or outpatient endoscopy center and generally follows these steps:
- Preparation:
Patients may receive a sedative or anesthesia to relax and minimize discomfort during the procedure. The throat is also numbed with a local anesthetic to ease the insertion of the endoscope.
- Insertion of the Endoscope:
The gastroenterologist carefully inserts the endoscope through the mouth and into the esophagus, stomach, and duodenum.
- Locating the Papilla:
The papilla of Vater, a small nipple-like structure where the common bile duct and pancreatic duct drain into the duodenum, is located using the endoscope.
- Contrast Injection:
A contrast medium (dye) is injected into the ducts to make them visible on X-ray images. Fluoroscopy is used to monitor the movement of the contrast medium.
- Imaging and Diagnosis:
X-ray images are captured in real-time to evaluate the structure and function of the bile ducts and pancreatic duct. If any abnormalities are detected, they can be further examined or treated during the same procedure.
- Therapeutic Procedures:
ERCP allows for various therapeutic interventions, such as removing gallstones, placing stents, widening strictures, or draining fluid collections. These procedures can alleviate symptoms and improve overall health.
- Completion:
Once the necessary diagnostic or therapeutic steps are completed, the endoscope is carefully removed.
The duration of an ERCP can vary but typically takes between 30 minutes to an hour. After the procedure, patients are monitored in a recovery area until the sedation wears off, and it is safe to be discharged.
Potential Risks and Complications of ERCP
While ERCP is generally considered a safe and effective procedure, like any medical intervention, it carries some risks and potential complications.
These can include:
- Pancreatitis: This is one of the most common complications of ERCP. Pancreatitis is inflammation of the pancreas and can range from mild to severe. It can cause abdominal pain, nausea, vomiting, and in severe cases, may require hospitalization. The risk of pancreatitis following ERCP varies but is generally around 5% to 10%. It is more common when therapeutic interventions, such as sphincterotomy (cutting of the sphincter), are performed during the procedure.
- Infection: Infections can occur in rare cases, either in the bile ducts or the pancreas. Bacterial infection can lead to symptoms such as fever, chills, and abdominal pain. Infection risk is minimized by following strict sterile techniques during the procedure.
- Bleeding: Although uncommon, bleeding can occur during or after ERCP, particularly if therapeutic procedures like sphincterotomy or stone removal are performed. Minor bleeding may resolve on its own, but significant bleeding may require additional interventions or surgery.
- Perforation: Perforation, or a tear in the digestive tract, is a rare but serious complication. It can lead to abdominal pain, infection, and the leakage of digestive contents into the abdominal cavity. Emergency surgery is usually necessary to repair a perforation.
- Allergic Reaction: Some patients may experience an allergic reaction to the contrast medium used during ERCP. Allergic reactions can range from mild skin rashes to more severe symptoms like difficulty breathing or anaphylaxis. The risk of a severe allergic reaction is relatively low.
- Complications Related to Anesthesia: Sedatives and anesthesia used during ERCP carry inherent risks, including respiratory depression, reduced oxygen levels, and reactions to medications. These risks are typically minimized by careful monitoring during the procedure.
- Other Risks: There is also a slight risk of complications such as blood clots, heart problems, or adverse reactions to medications used during ERCP.
It’s important to note that while these risks are associated with ERCP, the procedure is generally considered safe and effective when performed by experienced gastroenterologists or endoscopists.
Recovery and Aftercare
After an ERCP, patients are typically monitored for a brief period in a recovery area until they fully wake up from the sedation. It’s essential to arrange for a friend or family member to drive them home, as the sedatives can impair driving ability.
Patients may experience mild discomfort, bloating, or a sore throat for a day or two after the procedure, but these symptoms generally resolve on their own. If any complications or severe symptoms arise, such as persistent abdominal pain, fever, chills, or heavy bleeding, patients should contact their healthcare provider immediately.
Conclusion: The Power of ERCP in Gastroenterology
Endoscopic Retrograde Cholangiopancreatography (ERCP) is a powerful tool in the field of gastroenterology, offering both diagnostic and therapeutic capabilities.
By combining endoscopy and fluoroscopy, this procedure allows healthcare professionals to explore and treat conditions affecting the bile ducts, pancreas, and gallbladder with minimal invasiveness.
While ERCP can carry some risks and potential complications, it has greatly improved the accuracy of diagnoses and the effectiveness of treatments for a wide range of gastrointestinal conditions.
When performed by skilled and experienced gastroenterologists, ERCP can be a life-changing procedure that provides relief and improved quality of life for patients.

Contact Dr. Deetlefs
Dr Eduan prides himself on his ability to help his patients to the best of his ability by embracing good listening skills, effective communication, compassion and knowledge and skill honed during years of private gastroenterology practice.
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.