Understanding Fatty Liver Disease and How to Treat It
What is Fatty Liver Disease?
Fatty liver disease is a disease that effects the liver by replacing the liver cells with fat.
The liver is a very important organ in the body. It is the largest organ and plays an important role in digestion, the metabolism of cholesterol, bile production, and other important functions.
In fatty liver disease, the fat builds up inside the liver cells which makes the liver enlarged and non-functional.
The liver cells do not do their normal functions. The fat that builds up inside the liver cells are triglycerides.
Triglycerides are a type of fat found in the body. These fats are mostly stored in the liver. Fatty liver disease can lead to cirrhosis.
Cirrhosis is a type of liver disease that happens to people who have had fatty liver disease for a very long time. People who have cirrhosis may have liver failure or liver cancer.
Fatty liver disease is a disease that can lead to liver failure and liver cancer, which means that it is a very serious disease.
Fatty liver disease (also known as non-alcoholic fatty liver disease, or NAFLD) is a broad term that covers a lot of different conditions.
It’s not a specific disease, but a set of conditions that doctors treat differently depending on their cause.
NAFLD is a condition where too much fat builds up in the liver. The liver is an organ in the body that is responsible for filtering out toxins, producing proteins for the immune system, and breaking down nutrients from food.
When there is too much fat in the liver, the liver stops doing its job properly. Just like with alcohol, it’s not just people who drink a lot that can develop fatty liver disease.
A lot of people think NAFLD only affects people who are overweight or obese, but this isn’t true. If you eat a lot of fatty foods and do not get enough exercise to burn off the extra calories, you can develop fatty liver disease.
If you have fatty liver disease, also known as non-alcoholic fatty liver disease (NAFLD), it’s important to have a proper diagnosis. Once you’ve been diagnosed, you can start the treatment process.
This blog post will help you better understand fatty liver disease and how to treat it.
Signs and Symptoms of Fatty Liver Disease
The signs and symptoms of this condition vary according to the severity of the condition.
Because the liver is a vital organ, the signs and symptoms of fatty liver disease may vary from person to person.
They can range from mild to severe, depending on how much fat is in the liver. Some of the most common symptoms include:
- Fatigue
- Swelling
- Weight loss
- Abdominal pain
- Inability to sleep
- Fever
- Itching
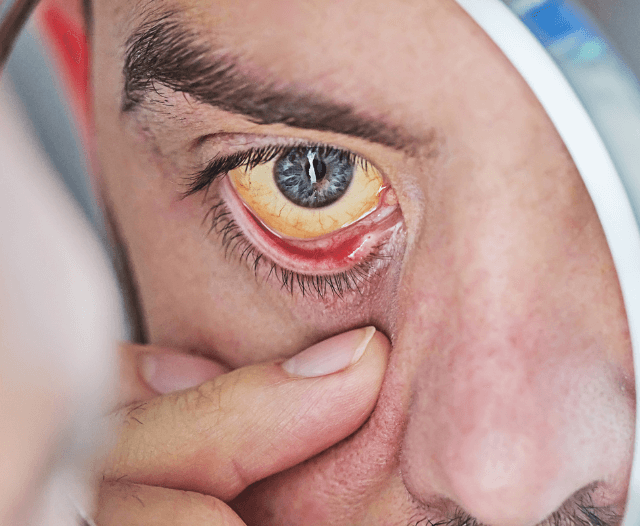
- Yellow skin or eyes
- Pain in the upper right belly
Usually, the symptoms of fatty liver disease are mild and easy to overlook. However, if left untreated, the condition can lead to more serious complications.
Should you experience any of the above-mentioned symptoms, it is advisable to contact your doctor for diagnosis.
Causes of Fatty Liver Disease
The liver is an important organ in the human body, and it is responsible for hundreds of functions, including metabolism, filtration, and blood production.
When the liver sustains damage, it is more likely to develop a fatty build-up, called a fatty liver.
The disease can be caused by a variety of factors, including:
- Obesity
- Type 2 diabetes
- Excessive alcohol consumption
- High cholesterol levels
While some cases of fatty liver are reversible, others can be more aggressive and lead to chronic liver damage and other long-term health problems.
Because of this, it is important to have a better understanding of the causes of fatty liver disease and what you can do to prevent or treat it.
How is Fatty Liver Disease Diagnosed?
Fatty liver disease is diagnosed by a combination of tests, including a physical examination, blood tests, and imaging tests.
The physical examination may reveal an enlarged liver. The blood tests may show elevated levels of liver enzymes. The imaging tests may show an accumulation of fat in the liver.
A liver biopsy may also be done to confirm the diagnosis.
In a liver biopsy, a small sample of liver tissue is removed and examined under a microscope.
The treatment of fatty liver disease depends on the underlying cause. If the cause is obesity or diabetes, weight loss and control of blood sugar levels are important.
If the cause is alcohol abuse, abstinence from alcohol is essential.
In some cases, liver transplant may be the only option.
Risk Factors of Fatty Liver Disease
There are many risk factors for fatty liver disease, including obesity, diabetes, high cholesterol, and high triglycerides.
Other risk factors include drinking too much alcohol, having hepatitis C, and taking certain medications.
Fatty liver disease can lead to serious health problems, including cirrhosis and liver cancer.
If you have any of these risk factors, it’s important to talk to your doctor about ways to reduce your risk.
How to Treat Fatty Liver Disease
There is no one-size-fits-all approach to treating fatty liver disease. The treatment plan will vary depending on the underlying cause of the condition.
For example, if the condition is due to obesity, weight loss may be recommended.
If the condition is due to excessive alcohol consumption, abstinence from alcohol may be recommended.
In some cases, medications may be necessary to manage the condition.
If you have been diagnosed with fatty liver disease, it is important to follow your treatment plan and make lifestyle changes as recommended by your doctor.
Doing so can help to improve your liver health and reduce your risk of developing serious complications.
How to Prevent Fatty Liver Disease?
There are a few things you can do to prevent fatty liver disease.
First, avoid drinking too much alcohol. If you do drink alcohol, be sure to stay hydrated by drinking plenty of water.
Second, eat a healthy diet that includes plenty of fruits, vegetables, and whole grains.
Avoid processed foods and sugary drinks.
Third, exercise regularly. This will help to keep your weight in check and your liver healthy.
Finally, if you have any other medical conditions, such as diabetes or high cholesterol, be sure to manage these conditions carefully.
By following these tips, you can help to prevent fatty liver disease.
Conclusion
Now that you have read a blog about fatty liver disease and how to treat it, you are one step closer to being an educated patient.
The liver is an important organ that helps to filter toxins from the body and to help with digestion. The liver helps to metabolize nutrients so that the body can use them to function properly.
Although fatty liver disease can be a serious condition, it is often treatable. If you have been diagnosed with fatty liver disease, work with your doctor to develop a treatment plan.
This may include lifestyle changes, such as eating a healthy diet and exercising regularly. In some cases, medications may also be necessary.
With proper treatment, you can improve your liver health and reduce your risk of complications.
If you are concerned about your liver health, talk to us today to book your appointment.
For further reading on the procedures we perform, please visit our website or contact Dr. Deetlefs.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.