IBS vs. IBD: Understanding the Differences and Treatment Options
Digestive discomfort is common, but when abdominal pain, bloating, or changes in bowel habits persist, many patients start to wonder what’s really going on. Two of the most common — and often confused — digestive disorders are Irritable Bowel Syndrome (IBS) and Inflammatory Bowel Disease (IBD).
Although their symptoms may overlap, these are very different conditions with distinct causes, diagnostic processes, and treatment approaches. Understanding these differences is key to finding effective relief — and knowing when to see a gastroenterologist like Dr. Eduan Deetlefs in Cape Town for expert evaluation and care.
What Is IBS?
Irritable Bowel Syndrome (IBS) is a functional gastrointestinal disorder, meaning there’s no visible inflammation or damage to the digestive tract. Instead, IBS involves a disturbance in how the gut functions, often related to hypersensitivity of the intestines or abnormal muscle contractions.
IBS affects the large intestine (colon) and can cause chronic digestive symptoms that fluctuate in intensity. It’s one of the most common GI conditions worldwide, affecting both men and women, often beginning in early adulthood.
Common Symptoms of IBS:
- Recurrent abdominal pain or cramping
- Bloating or excessive gas
- Changes in bowel habits — diarrhea, constipation, or alternating between both
- A feeling of incomplete bowel emptying
- Mucus in the stool
- Relief of pain after a bowel movement
IBS symptoms are often triggered by diet, stress, or hormonal changes, and they may come and go over time. Importantly, IBS does not cause intestinal damage, bleeding, or weight loss — these signs usually indicate another condition.

What Is IBD?
Inflammatory Bowel Disease (IBD) refers to chronic, immune-mediated inflammation of the digestive tract. Unlike IBS, IBD causes visible damage to the intestinal lining, which can lead to serious complications if untreated.
There are two main types of IBD:
- Crohn’s Disease – can affect any part of the digestive tract from the mouth to the anus, often in “patchy” segments.
- Ulcerative Colitis – affects only the colon and rectum, causing continuous inflammation and ulcers in the intestinal lining.
IBD is an autoimmune condition, meaning the body’s immune system mistakenly attacks healthy cells in the gut, causing inflammation and tissue injury.

Common Symptoms of IBD:
- Persistent diarrhea (sometimes with blood or mucus)
- Abdominal pain and cramping
- Unintended weight loss
- Fatigue
- Loss of appetite
- Blood in the stool
- Fever or joint pain in severe flare-ups
Because IBD causes real inflammation, it can lead to complications such as intestinal strictures, fistulas, abscesses, or increased risk of colon cancer — making early diagnosis and treatment essential.
🔍 IBS vs. IBD: Key Differences at a Glance
| Feature | IBS (Irritable Bowel Syndrome) | IBD (Inflammatory Bowel Disease) |
| Type of condition | Functional disorder (no visible damage) | Autoimmune inflammatory disease |
| Affected areas | Large intestine (colon) | Any part of GI tract (Crohn’s) or colon/rectum (Ulcerative Colitis) |
| Cause | Gut hypersensitivity, stress, diet, hormonal factors | Immune system attacking intestinal tissue |
| Inflammation present? | ❌ No | ✅ Yes |
| Symptoms | Bloating, pain, diarrhea/constipation, mucus | Bloody diarrhea, pain, fatigue, weight loss |
| Complications | None (does not cause damage) | Intestinal damage, strictures, cancer risk |
| Diagnosis | Clinical history, exclusion of other diseases | Colonoscopy, biopsies, blood/stool tests, imaging |
| Treatment goal | Symptom management | Inflammation control and remission |
| Seriousness | Chronic but not life-threatening | Can be serious or life-threatening if untreated |
🧠 Understanding the Causes
Causes of IBS
The exact cause of IBS is not fully understood, but several factors are thought to contribute:
- Abnormal gut motility: Muscles in the intestines contract too quickly or too slowly.
- Visceral hypersensitivity: The nerves in the gut are overly sensitive to stretching or movement.
- Gut-brain axis dysfunction: Stress and anxiety can directly affect gut function through nerve signals.
- Dietary triggers: Fatty foods, caffeine, dairy, and artificial sweeteners may worsen symptoms.
- Post-infectious IBS: Some people develop IBS after a bacterial or viral infection.
Causes of IBD
IBD is more complex, involving a mix of immune, genetic, and environmental factors:
- Immune system dysfunction: The body mistakenly attacks the intestinal lining.
- Genetics: A family history of IBD increases risk.
- Gut microbiome imbalance: Certain bacteria may trigger inflammation.
- Environmental factors: Smoking, diet, and infections may contribute.

🧪 Diagnosing IBS vs. IBD
Because their symptoms overlap, a proper diagnosis is essential.
Diagnosing IBS
IBS is usually diagnosed by excluding other conditions. Gastroenterologists use the Rome IV Criteria, which include:
- Abdominal pain at least once per week for the last 3 months
- Pain related to bowel movements or changes in stool frequency/consistency
Tests may include:
- Blood tests to rule out celiac disease or anemia
- Stool tests to check for inflammation
- Colonoscopy (if red-flag symptoms like bleeding or weight loss are present)
Diagnosing IBD
IBD requires more direct evaluation of inflammation and damage. Dr. Deetlefs may recommend:
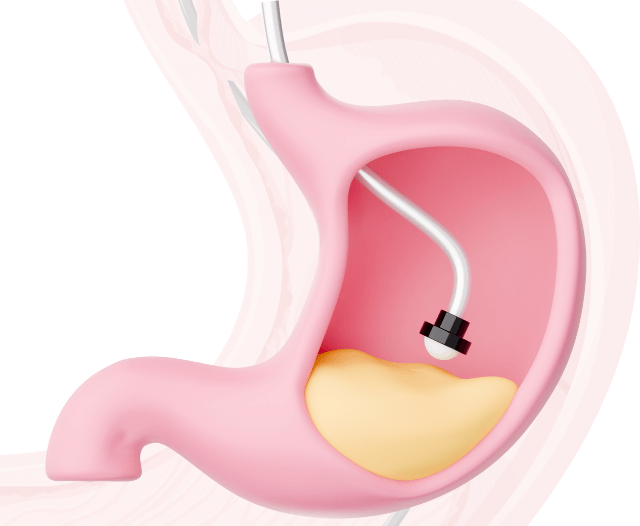
- Colonoscopy or gastroscopy – to view and biopsy inflamed tissue
- Blood tests – checking for anemia, infection, or inflammation markers
- Stool tests (calprotectin or lactoferrin) – to measure intestinal inflammation
- Imaging (CT or MRI enterography) – to visualize small bowel involvement in Crohn’s disease

💊 Treatment Options for IBS and IBD
IBS Treatment
Because IBS is functional, treatment focuses on symptom control and lifestyle modification.
- Dietary Management
- Low-FODMAP diet: Eliminating fermentable carbohydrates that cause gas and bloating.
- High-fiber diet: Helps relieve constipation (for IBS-C).
- Avoiding trigger foods: Caffeine, spicy food, alcohol, and processed meals.
- Stress and Lifestyle
- Regular exercise and mindfulness can reduce gut-brain tension.
- Good sleep hygiene and stress reduction techniques (yoga, deep breathing).
- Medications
- Antispasmodics: Reduce cramping.
- Antidiarrheals or laxatives: For bowel habit regulation.
- Low-dose antidepressants: Modulate gut nerve sensitivity.
- Probiotics: Support healthy gut flora.
IBD Treatment
IBD requires a more targeted medical approach to reduce inflammation and prevent long-term damage.
- Anti-Inflammatory Medications
- Aminosalicylates (5-ASA): Reduce inflammation in the colon.
- Corticosteroids: Used short-term for acute flare-ups.
- Immune System Suppressors
- Azathioprine or methotrexate: Help reduce immune overactivity.
- Biologic Therapies
- Advanced treatments that target specific inflammatory pathways (e.g., TNF inhibitors, integrin blockers).
- Biologics have revolutionized IBD management, offering long-term remission and mucosal healing.
- Nutritional Support
- Ensures patients maintain healthy weight and nutrient levels during flare-ups.
- Endoscopic or Surgical Interventions
- Endoscopic dilatation may treat strictures caused by Crohn’s disease.
- Surgery may be necessary for severe cases or complications such as bowel obstruction or perforation.

⏰ When to See a Gastroenterologist
While mild digestive discomfort can often be managed with diet, persistent or severe symptoms require medical evaluation.
You should see a gastroenterologist like Dr. Eduan Deetlefs if you experience:
- Blood in your stool
- Persistent diarrhea or constipation
- Severe or unexplained abdominal pain
- Unexplained weight loss or fatigue
- Symptoms that do not improve with over-the-counter treatments
- A family history of IBD or colon cancer
Early consultation allows for accurate diagnosis and tailored treatment, improving both comfort and long-term gut health.
👨⚕️ About Dr. Eduan Deetlefs – Cape Town Gastroenterologist
Dr. Eduan Deetlefs is a highly experienced gastroenterologist based in Cape Town, specializing in the diagnosis and management of gastrointestinal disorders such as IBS, IBD, acid reflux, Crohn’s disease, ulcerative colitis, and liver conditions.
He provides a comprehensive range of diagnostic procedures, including colonoscopy, gastroscopy, endoscopic dilatation, and stent placement, using advanced technology to ensure accurate diagnosis and effective treatment.
If you’re struggling with chronic digestive symptoms or uncertain whether your condition is IBS or IBD, book a consultation with Dr. Deetlefs for expert evaluation and compassionate care.
📍 Visit: www.gidoc.co.za
📞 Call: 021 202 0626
📧 Email: info@gidoc.co.za

✅ Takeaway
While IBS and IBD may sound similar, they are fundamentally different in cause, severity, and management. IBS affects how your gut works, while IBD affects its structure. Both can significantly impact quality of life — but with expert guidance and individualized care, patients can achieve relief, stability, and confidence in managing their digestive health.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.