Understanding Common Gastroenterology Procedures and Conditions
Gastroenterology is a branch of medicine focused on the digestive system and its disorders.
This field encompasses the diagnosis, treatment, and prevention of conditions affecting the gastrointestinal (GI) tract, which includes the esophagus, stomach, small intestine, colon, rectum, pancreas, gallbladder, bile ducts, and liver.
This article will provide an in-depth look at common gastroenterology procedures and conditions, aiming to educate and inform readers about the importance of digestive health.
Common Gastroenterological Conditions
Gastroesophageal Reflux Disease (GERD)
GERD is a chronic condition where stomach acid frequently flows back into the esophagus, leading to irritation. Symptoms include heartburn, regurgitation, and difficulty swallowing. Lifestyle changes, medications, and sometimes surgery are used to manage GERD.
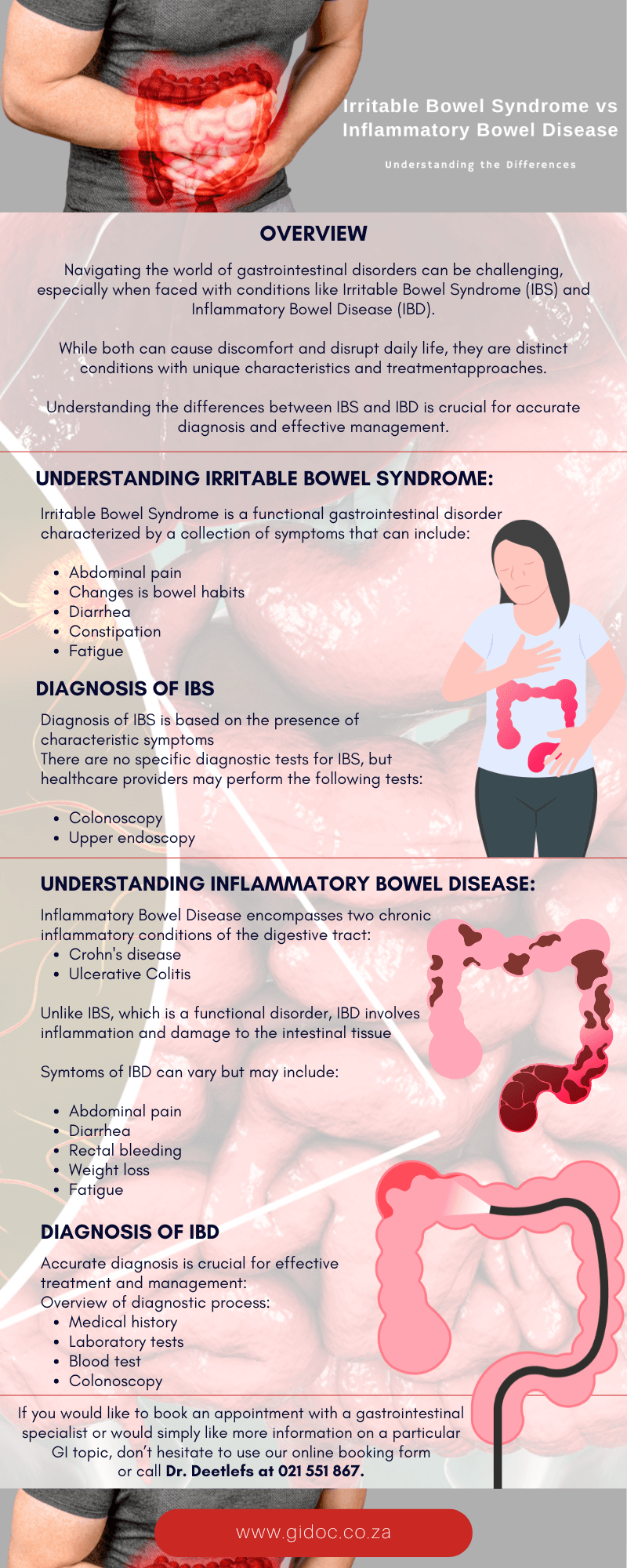
Irritable Bowel Syndrome (IBS)
IBS is a common disorder that affects the large intestine. It causes symptoms such as cramping, abdominal pain, bloating, gas, diarrhea, and constipation. Managing IBS typically involves dietary changes, stress management, and medications.

Inflammatory Bowel Disease (IBD)
IBD includes conditions like Crohn’s disease and ulcerative colitis, which involve chronic inflammation of the digestive tract. Symptoms include severe diarrhea, pain, fatigue, and weight loss. Treatment often involves medication to reduce inflammation and, in severe cases, surgery.
Celiac Disease
Celiac disease is an autoimmune disorder where ingestion of gluten leads to damage in the small intestine. Symptoms include diarrhea, bloating, and weight loss. The primary treatment is a strict gluten-free diet.
Gallstones
Gallstones are hardened deposits of digestive fluid that can form in the gallbladder. They can cause pain, nausea, and serious complications if they block a bile duct. Treatment may involve medication to dissolve the stones or surgery to remove the gallbladder.
Hepatitis
Hepatitis is inflammation of the liver, often caused by viral infections (hepatitis A, B, and C), but also by alcohol, drugs, or autoimmune diseases. Symptoms include jaundice, fatigue, and abdominal pain. Treatment varies depending on the type and cause of hepatitis.
Pancreatitis
Pancreatitis is inflammation of the pancreas, which can be acute or chronic. Symptoms include upper abdominal pain, nausea, and vomiting. Treatment may involve fasting, pain management, and addressing the underlying cause.
Colon Cancer
Colon cancer begins in the large intestine (colon). It typically starts as benign polyps that can become cancerous over time. Symptoms include changes in bowel habits, blood in the stool, and unexplained weight loss. Screening and early detection through colonoscopy can significantly improve outcomes.

Common Gastroenterological Procedures
Endoscopy
Endoscopy involves inserting a flexible tube with a camera (endoscope) into the GI tract to diagnose and sometimes treat conditions.
Types of endoscopy include:
- Upper Endoscopy (Esophagogastroduodenoscopy or EGD): Examines the esophagus, stomach, and duodenum.
- Colonoscopy: Examines the colon and rectum.
- Capsule Endoscopy: Involves swallowing a small capsule with a camera to examine the small intestine.
Colonoscopy
A colonoscopy is a procedure to examine the inner lining of the colon and rectum using a long, flexible tube with a camera. It is used for screening and diagnosing conditions like colorectal cancer, polyps, and inflammatory bowel disease. Biopsies can also be taken during the procedure.
Endoscopic Retrograde Cholangiopancreatography (ERCP)
ERCP is a procedure used to diagnose and treat problems in the liver, gallbladder, bile ducts, and pancreas. It combines endoscopy and X-ray to visualize these organs and can also involve therapeutic interventions like removing stones or placing stents.
Endoscopic Ultrasound (EUS)
EUS combines endoscopy and ultrasound to obtain detailed images of the digestive tract and surrounding tissues. It is used to diagnose and stage cancers, evaluate pancreatic and biliary diseases, and guide fine-needle aspiration for biopsy.
Flexible Sigmoidoscopy
Similar to a colonoscopy, flexible sigmoidoscopy examines the rectum and lower part of the colon using a shorter tube with a camera. It is used for screening and diagnosing conditions affecting the lower GI tract.
Liver Biopsy
A liver biopsy involves taking a small sample of liver tissue for examination under a microscope. It is used to diagnose liver diseases, monitor treatment, and assess liver damage.
Breath Tests
Breath tests can diagnose conditions like small intestinal bacterial overgrowth (SIBO), lactose intolerance, and Helicobacter pylori infection. They involve analyzing the breath after ingesting specific substances.
Barium Swallow and Barium Enema
These imaging tests use a contrast material (barium) to visualize the upper GI tract (barium swallow) or the colon (barium enema) on X-rays. They help diagnose structural abnormalities and motility disorders.

Preventive Measures and Lifestyle Changes
Maintaining digestive health is crucial for preventing GI disorders and complications.
Here are some general tips:
Diet
Fiber-Rich Foods: Include plenty of fruits, vegetables, whole grains, and legumes in your diet to promote healthy digestion.
Hydration: Drink enough water to keep the digestive system functioning smoothly.
Limit Fatty Foods: Reduce intake of high-fat foods that can slow digestion and cause discomfort.
Avoid Trigger Foods: Identify and avoid foods that trigger symptoms of conditions like GERD, IBS, and food intolerances.
Exercise
Regular Physical Activity: Engage in at least 150 minutes of moderate aerobic exercise or 75 minutes of vigorous exercise per week. Activities like walking, cycling, and swimming are beneficial for digestion.
Strength Training: Include strength training exercises at least two days a week to maintain muscle mass and support overall health.

Avoid Smoking and Excessive Alcohol
Smoking and excessive alcohol consumption can damage the digestive system and increase the risk of various GI disorders.
Stress Management
Mind-Body Practices: Practices such as yoga, meditation, and tai chi can reduce stress and improve digestive health.
Counseling and Therapy: Psychological therapies, including cognitive-behavioral therapy (CBT), can be effective for managing conditions like IBS and stress-related digestive issues.
Regular Screenings
Colorectal Cancer: Begin screening for colorectal cancer at age 50 (or earlier if there is a family history) and continue at regular intervals based on the chosen method and risk factors.
Liver Health: Regular monitoring of liver function tests and hepatitis screenings for those at risk can help in early detection and management of liver diseases.
Gastrointestinal Health: Regular check-ups with a gastroenterologist can help in early detection and management of GI conditions, especially for individuals with symptoms or a family history of GI diseases.

Conclusion
Understanding the various gastroenterological conditions, their symptoms, and the available diagnostic and treatment options is essential for maintaining optimal digestive health.
By adopting preventive measures such as a balanced diet, regular exercise, stress management, and routine screenings, individuals can significantly reduce their risk of developing GI disorders and improve their overall well-being.
If you experience persistent digestive symptoms or have a family history of GI conditions, consulting a gastroenterologist is crucial. Early diagnosis and tailored treatment plans can lead to better health outcomes and a higher quality of life.
Remember, your digestive health plays a vital role in your overall health, and taking proactive steps to maintain it can lead to long-term benefits.
Gi Doc Capetown is a practice founded to provide medical solutions in the area of gastroenterology.
Over the years, Dr Eduan Deetlefs has earned the reputation of a trusted health expert providing consultative, diagnostic, and therapeutic endoscopic and related services to patients in
Cape Town and beyond.
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.