Understanding Ulcerative Colitis
Overview of Ulcerative Colitis
Ulcerative colitis is a chronic inflammatory bowel disease that primarily affects the colon and rectum. The condition causes inflammation and sores (ulcers) to develop on the inner lining of the large intestine, leading to symptoms such as diarrhea, abdominal pain, and rectal bleeding.
The exact cause of ulcerative colitis is not known, but it is thought to be an autoimmune disorder in which the body’s immune system mistakenly attacks the lining of the colon and rectum.
Other factors that may contribute to the development of ulcerative colitis include genetics, environmental factors, and an imbalance of gut bacteria.
Symptoms of ulcerative colitis can vary in severity and may include diarrhea, bloody stools, abdominal pain and cramping, fatigue, weight loss, and fever.
Flares of the disease can be unpredictable and may be triggered by factors such as stress, infections, or changes in diet.
Treatment for ulcerative colitis typically involves medications to reduce inflammation and manage symptoms, such as corticosteroids, immunosuppressants, and biologics.
In this blog, we will delve into the topic of ulcerative colitis, a chronic inflammatory bowel disease that affects the colon and rectum.
Symptoms
The symptoms of ulcerative colitis can vary from person to person, and they may range from mild to severe.
Some of the most common symptoms of UC include:
- Diarrhea, often with blood or pus
- Abdominal pain and cramping
- Urgency to have a bowel movement
- Inability to have a bowel movement despite urgency
- Rectal pain and bleeding
- Fatigue
- Loss of appetite and weight loss
- Anemia
Causes
The exact cause of ulcerative colitis is unknown, but it is thought to be a result of a combination of genetic, environmental, and immunological factors.
People with a family history of UC are at a higher risk of developing the disease.
Other factors that may contribute to the development of UC include a compromised immune system, bacterial or viral infections, and stress.
Diagnosis
The diagnosis of ulcerative colitis involves a combination of medical history, physical examination, and diagnostic tests.
A healthcare provider will ask about the patient’s symptoms, medical history, and family history of IBD.
A physical exam may also be conducted to check for signs of inflammation in the abdomen.
Diagnostic tests that may be used to diagnose UC include:
Blood tests to check for signs of inflammation or infection
Blood tests can be useful in the diagnosis and management of ulcerative colitis (UC).
While there is no one specific blood test that can definitively diagnose UC, blood tests can help rule out other conditions that may have similar symptoms and help monitor disease activity and response to treatment.
Some of the tests that may be ordered for UC include:
- Complete blood count (CBC):
This test measures the levels of different types of blood cells, including red blood cells, white blood cells, and platelets. In UC, the CBC can show signs of anemia (low red blood cell count) or inflammation (elevated white blood cell count). - Stool tests to check for blood, infections, or parasites
- CT scan or MRI to evaluate the extent of inflammation and complications
- Colonoscopy to visualize the colon and take tissue samples for biopsy
Colonoscopy Explained
Colonoscopy is a medical procedure that allows healthcare providers to visualize the inside of the colon and rectum using a flexible, lighted tube called a colonoscope.
The procedure is used to screen for colon cancer, diagnose and treat various gastrointestinal conditions, and monitor the effectiveness of treatment.
During a colonoscopy, the patient lies on their side while the colonoscope is inserted into the rectum and advanced through the colon.
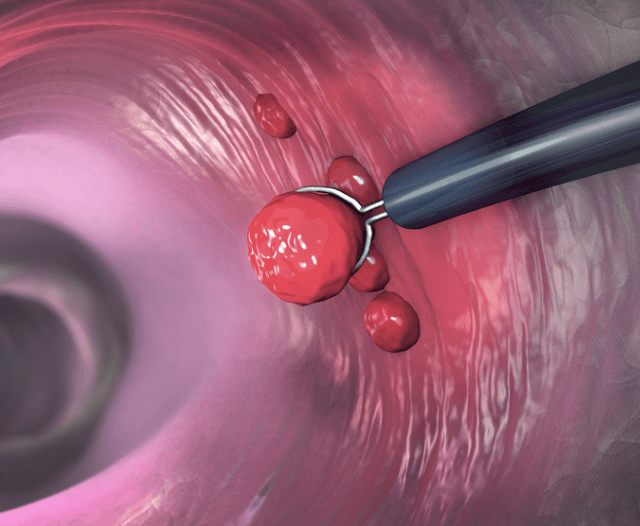
The colonoscope has a tiny camera on the end, which sends images to a monitor that the healthcare provider uses to examine the colon lining for abnormalities such as polyps, inflammation, or cancerous growths.
Before a colonoscopy, patients must follow a special diet and take laxatives to cleanse the colon.
They may also receive sedation or anesthesia to help them relax and reduce discomfort during the procedure.
If any abnormalities are found during the colonoscopy, the healthcare provider may take a biopsy or remove the abnormal tissue for further testing.
The removed tissue is then sent to a lab for analysis to determine if it is cancerous or benign.
Although colonoscopy is generally considered a safe procedure, there are some risks, including bleeding, infection, and perforation of the colon.
It is important to discuss any concerns with the healthcare provider before the procedure.
In summary, colonoscopy is a procedure that allows healthcare providers to examine the colon and rectum for abnormalities using a colonoscope.
The procedure is used to screen for conditions and diagnose and treat gastrointestinal conditions, and monitor treatment effectiveness.
Patients must prepare for the procedure by following a special diet and taking laxatives to cleanse the colon.
If abnormalities are found, a biopsy or removal of tissue may be necessary for further testing.
While generally safe, there are some risks associated with the procedure.
Treatment
The treatment of ulcerative colitis may involve medications and lifestyle changes.
The goals of treatment are to reduce inflammation, manage symptoms, and prevent complications.
Medications that may be used to treat UC include:
- Aminosalicylates (5-ASAs) to reduce inflammation
- Corticosteroids to reduce inflammation
- Immunosuppressants to suppress the immune system
- Biologic therapies to target specific proteins involved in inflammation
- Lifestyle changes
- Eating a healthy and balanced diet
- Staying hydrated
- Getting regular exercise
- Reducing stress
- Quitting smoking
In some cases, surgery may be necessary to remove the affected part of the colon or rectum.
Traveling with Ulcerative Colitis:
Traveling can be stressful for people with ulcerative colitis, as it can disrupt daily routines and access to medical care.
It is important to stay calm during travelling, keep an emergency kit with you and stay hydrated.
Alternative Therapies for Ulcerative Colitis:
While conventional medical treatments are often effective for managing ulcerative colitis, some people may seek out alternative therapies, such as acupuncture or herbal remedies.
The Latest Research on Ulcerative Colitis:
Ulcerative colitis is a rapidly evolving field, with new research and treatments emerging all the time.
In this blog post, you could highlight some of the latest research on ulcerative colitis, including advances in genetics, immunology, and microbiome research.
Conclusion:
In conclusion, ulcerative colitis is a chronic inflammatory disease that affects the colon and rectum.
It can cause a range of uncomfortable symptoms. Although there is no known cure for ulcerative colitis, there are a variety of treatment options available to manage the symptoms and improve quality of life for patients.
It is important for individuals with ulcerative colitis to work closely with their healthcare providers to develop a personalized treatment plan that addresses their specific symptoms and needs. This may involve a combination of medications, lifestyle changes, and dietary modifications.
Furthermore, it is essential to stay up to date with regular check-ups and monitoring to ensure that the disease is under control and to prevent the development of serious complications, such as colon cancer.
Living with ulcerative colitis can be challenging, but with proper care and management, it is possible to lead a healthy and fulfilling life.
For any additional information regarding a Colonoscopy procedure, it’s best to find a trusted and experienced Gastroenterologist who can answer your questions clearly, recommend appropriate solutions, and perform tests with precision and expertise.
Dr. Deetlefs has earned the reputation of a trusted health expert providing consultative, diagnostic, and therapeutic endoscopic and related services to patients in Cape Town and beyond.
Dr Eduan prides himself on his ability to help his patients to the best of his ability by embracing good listening skills, effective communication, compassion and knowledge and skill honed during years of private gastroenterology practice.
If you would like to book an appointment with a gastrointestinal (GI) specialist or would simply like more information on a particular GI topic, don’t hesitate to use our online booking form
or call Dr. Deetlefs at 021 551 867.
DISCLAIMER: PLEASE READ CAREFULLY
The information on this website is to provide general guidance. In no way does any of the information provided reflect definitive medical advice and self-diagnoses should not be made based on information obtained online. It is important to consult a Gastroenterologist or medical doctor regarding ANY and ALL symptoms or signs including, but not limited to: abdominal pain, haemorrhoids or anal / rectal bleeding as it may a sign of a serious illness or condition. A thorough consultation and examination should ALWAYS be performed for an accurate diagnosis and treatment plan. Be sure to call a physician or call our office today and schedule a consultation.
© Dr. Eduan Deetlefs, Registered Gastroenterologist, GI Doc Cape Town
Our website information is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a doctor about your specific condition. Only a trained physician can determine an accurate diagnosis and proper treatment.